Enhance your health with free online physiotherapy exercise lessons and videos about various disease and health condition
PIVD and Herniated Disc Exercises
What is a P.I.V.D or prolapsed disc ?
The term PIVD /prolapsed intervertebral disc means the protrusion or extrusion of the nucleus pulposus through a rent in the annulus fibrosus.
It has a four stages-
- Bulging- At this early stage, the disc is stretched and doesn't completely return to its normal shape when pressure is relieved. It retains a slight bulge at one side of the disc. Some of the inner disc fibres could be torn and the soft jelly ( nucleus pulposus ) is spiling outwards into the disc fibres but not out of the disc.
- Protrusion- At this stage, the bulge is very prominent and the soft jelly centre has spilled out to the inner edge of the outer fibres, barely held in by the remaining disc fibres.
- Extrusion- In the case of a herniated spinal disc, the soft jelly has completely spilled out of the disc and now protruding out of the disc fibres.
- Sequestration- Here some of the jelly material is breaking off away from the disc into the surrounding area.
prolapsed disc (commonly called a 'slipped disc'), a disc does not actually 'slip'. What happens is that part of the inner softer part of the disc (the nucleus pulposus) bulges out (herniates) through a weakness in the outer part of the disc. A PIVD /prolapsed disc is sometimes called a herniated disc. The bulging disc may press on nearby structures such as a nerve coming from the spinal cord. Some inflammation also develops around the prolapsed part of the disc. Any disc in the spine can prolapse. However, most prolapsed discs occur in the lumbar part of the spine (lower back). The size of the prolapse can vary. As a rule, the larger the prolapse, the more severe the symptoms are likely to be.
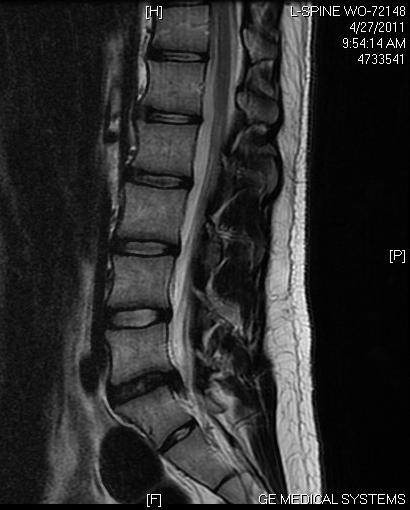
Understanding the back
The spine is made up of many bones called vertebrae. These are roughly circular and between each vertebra is a 'disc'. The discs are made of strong 'rubber-like' tissue which allows the spine to be fairly flexible. A disc has a stronger fibrous outer part, and a softer jelly-like middle part called the nucleus pulposus. The spinal cord, which contains the nerves that come from the brain, is protected by the spine. Nerves from the spinal cord come out from between the vertebrae to take and receive messages to various parts of the body. Strong ligaments attach to the vertebrae. These give extra support and strength to the spine. Various muscles also surround, and are attached to, various parts of the spine.
Anatomy of Intervertebral discs
Intervertebral Discs are soft, rubbery pads found between the hard bones (vertebrae) that make up the spinal column. The spinal canal is a hollow space in the middle of the spinal column that contains the spinal cord and other nerve roots. The discs between the vertebrae allow the back to flex or bend. Discs also act as shock absorbers. Normal anatomy of lumbar spine. Discs in the lumbar spine (low back) are composed of a thick outer ring of cartilage (annulus fibrosus) and an inner gel-like substance (nucleus pulposus). In the cervical spine (neck), the discs are similar but smaller in size. Two layers of cartilage which cover top and bottom aspect of each disc called a vertebral end plate. Its separate the disc from the adjacent vertebral body.
nucleus pulposus It is semi fluid mass of mucoid material seems like a toothpaste. It consist of few cartilage cells and irregular arranged collagen fibers. The fluid nature of nucleus pulposus allowed it to be deformed under pressure. The nucleus attempt to deformed and will there by transmit the applied pressure in all direction.
annulus fibrosus The annulus fibrosus consist of collagen fibers. The collagen fibers are arranged in between 10 to 20 sheets called lamellae. These are arranged in concentric rings that surround the nucleus pulposus. They are thick in anterior and lateral portion of the annulus but posteriorly they are finer and more tightly packed. The collagen fibers lie parellel to each other. Posterior portion of annulus fibrosus is innervated by fibres of sinuvertebral nerve (branch of dorsal root ganglion). Irritation of the sinuvertebral nerve is responsible for axial back pain.
Vertebral End Plates Each vertebral end plate is a layer of cartilage about 0.6-1 mm thick. Covers the area on the vertebral area encircled by the ring apophysis. Nucleus pulposus is entirely covered but annulus fibrosus is only 66% covered by the end plates.
Types of herniation
- central
- paramedial
- lateral
What causes a PIVD ?
- Heavy manual labour
- Repetitive lifting and twisting
- Postural stress
- obesity
- Poor and inadequate strength of the trunk
- Sitting for long hours
- increasing age (a disc is more likely to develop a weakness with increasing age)
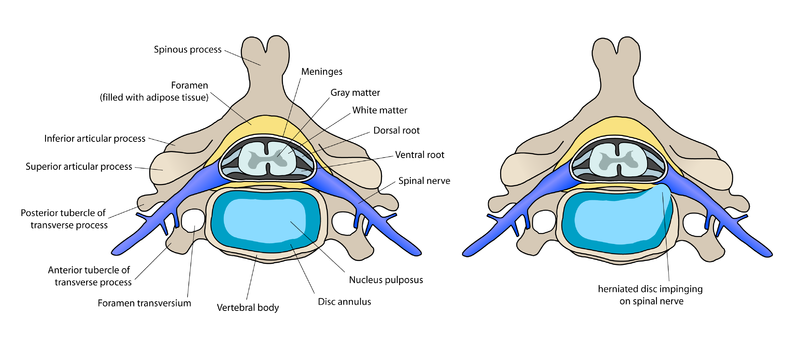
What are the symptoms of PIVD ?
Lower Back /Lumbar Herniated Disc Symptoms
- Severe low-back pain
- Pain radiating to the buttocks, legs, and feet
- Pain made worse with coughing, straining or laughing
- Muscle spasm
- Tingling or numbness in legs or feet
- Muscle weakness or atrophy in later stages
- Loss of bladder or bowel control in case of cauda equina syndrome
Some people do not have symptoms of PIVD Research studies where routine back scans have been done on a large number of people have shown that some people have a PIVD without any symptoms. It is thought that symptoms mainly occur if the prolapse causes pressure or irritation of a nerve. This does not happen in all cases. Some prolapses may be small, or occur away from the nerves and cause minor, or no symptoms.
Neck /Cervical Herniated Disc Symptoms
- Arm muscle weakness
- Deep pain near or over the shoulder blades on the affected side
- Increased pain when bending the neck or turning head to the side
- Pain made worse with coughing, straining or laughing
- Neck pain, especially in the back and sides along with spasm
- Burning pain radiating to the shoulder, upper arm, forearm, and rarely the hand, fingers or chest
- Tingling (a "pins-and-needles" sensation) or numbness in one arm
Cauda equina syndrome - rare, but an emergency
Cauda equina syndrome is a particularly serious type of nerve root problem that can be caused by a prolapsed disc. This is a rare disorder where the nerves at the very bottom of the spinal cord are pressed on. This syndrome can cause low back pain plus: problems with bowel and bladder function (usually unable to pass urine), numbness in the 'saddle' area (around the anus), and weakness in one or both legs. This syndrome needs urgent treatment to preserve the nerves to the bladder and bowel from becoming permanently damaged. See a doctor immediately if you develop these symptoms.
Bulging Discs vs. Herniated Discs
The primary difference between bulging discs and herniated discs are whether they are contained or non-contained:
A contained disc- such as a bulging disc, has not broken through the outer wall of the intervertebral disc, which means the nucleus pulposus remains contained within the annulus fibrosus.
A non-contained disc- such as a herniated or ruptured disc, has either partially or completely broken through the outer wall of the intervertebral disc. A bulging disc may be a precursor to a herniation. The disc may protrude into the spinal canal without breaking through the disc wall. The gel-like interior (nucleus pulposus) does not leak out. The disc remains intact except a small bubble appears on the outside of the disc. When a disc herniates, the contents may compress the spinal cord or the spinal nerve roots.To complicate matters, sometimes fragments from the annulus (the outer disc wall) may breakaway from the parent disc and drift into the spinal canal.
Do I need any tests for PIVD ?
Special Tests for PIVD-
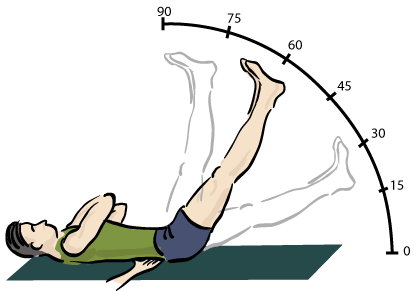
- SLR test
- Laesegue test
- Bowstring test
- Femoral stretch test
Your doctor will normally be able to diagnose a PIVD from the symptoms and by examining you. (It is the common cause of sudden back pain with nerve root symptoms). In most cases of PIVD, tests such as x-rays or scans my be advised if symptoms persist. In particular, an MRI scan can show the site and size of a prolapsed disc. This information is needed if treatment with surgery is being considered.
PIVD Treatment
1.Conservative Management-
a) Rest: Rest and Anti-inflammatory and analgesics.
b) Reduction: Continue bed rest and traction for 2 weeks may reduce the herniation in over 90% cases. If no improvement with rest and traction, epidural injection of corticosteroid and local anaesthetic are given.
c) Chemonucleolysis: dissolution of the Nucleus Pulposus by percutaneous injection of a proteolytic enzyme (chymopapain). This enzyme has the property of dissolving fibrous and cartilaginous tissue.
2.Operative Management-
Indications for operative removal of disc.
i) cauda equina compression syndrome that does not clear up with 6 hours of starting bed rest and traction (emergengy).
ii) Neurological deterioration while under conservative management.
iii) Persistant pain and signs of sciatic tension after 3 weeks of conservative treatment.
The disc is removed by following techniques.
a) Hemilaminectomy/Partial laminectomy- Part of the lamina and ligamentum flavum on one side is removed, taking great care not to damage the facet joint.
b) Laminectomy- Laminae on both sides with spinous process are removed. Such wide exposure is required for big, central disc producing cauda equina syndrome.
c) Microdiscectomy- done with an operating microscope. Exposure is very limited. Morbidity and hospitalisation is less.
d) Fenestration- Ligamentum flavum bridging the two adjacent laminae is excised and spinal canal at affected level exposed.
e) Laminotomy- In addition to fenestration, a hole is made in the lamina for wider exposure.
Physical Therapy Management in PIVD
Before planning the treatment, determine the position of comfort or symptom reduction i.e FUNCTIONAL POSITION. The patient may have...
a) Extension bias: Patient's symptoms are lessened in position of extension (bending back) and provoked in flexion (bending forwards) e.g PIVD.
b) Flexion bias: Patient's symptoms are lessened in position of spinal flexion (bending forwards) and provoked in spinal extension (bending backwards) e.g spinal stenosis, spondylolisthesis.
Spinal Extension (bending back) is contraindicated if:
i) when no position or movement decreases or centralizes the pain.
ii) when saddle anaesthesia and/or urinary incontinence is present (could indicate spinal cord or cauda equina lesion due to large central disc herniation).
iii) when patient is in such extreme pain that he rigidly holds the body immobile.
Spinal flexion (bending forward) is contraindicated if:
i) when extension relieves the symptoms.
ii) when flexion increases or peripheralises the symptoms.
ACUTE PHASE:
Aims:
a) To relieve pain.
b) To promote muscle relaxation.
c) To relieve inflammation and pressure against the pain sensitive or neurologic structures.
d) patient education.
e) prevention.
Physical Therapy Management in Acute Phase of PIVD:
a) CONTROLLED REST- is recommended i.e rest in the form of-
*Posture and activity modification- Avoid flexed postures, sitting for long duraton, bending or lifting activities, asymmetric postures ( flexion and rotation). All these increase the disc pressure.
*Local support in the form of corset (lumbosacral belt), abdominal binder, tape etc. These measures will enhance healing and prevent reinjury to the healing disc. Within 10 days fibrin is laid down. If spine is maintained in lordosis, the annulus will heal in shortened position and nucleus will be retained centrally.
*If symptoms are severe, bed rest (maximum for 2 days) on a hard bed is indicated with short periods of walking at regular intervals ( with corset). Walking promotes lumbar extension and stimulates fluid mechanics to help reduce swelling in the disc/connective tissues.
*If patient presents with inability to straighten up, make the patient lie prone with 2-3 pillows under the abdomen. As the pain subsides, remove the pillows and prop up the trunk by placing pillows under the thorax. By this nucleus pulposus is shifted forwards and relieves pain and gains a lordosis.
b) MODALITIES TO REDUCE PAIN AND SPASM-
*Cryotherapy: reduces muscle spasm and inflammation in acute phase.
*TENS: relieves pain in both acute and chronic phases.
*US: as phonophoresis increases extensibility of connective tissues
*Moist heat: used as an adjunct before applying specialised techniques to decrease muscle spasm.
*SWD- pulsed SWD in acute condition and continuous SWD in chronic cases.
*IFT
*Soft tissue manipulation- to reduce local muscle spasm and induce relaxation.
*Traction- may be beneficial to relieve nerve root compression and radiculopathy or paraesthesias in the acute phase of PIVD. Reduces nuclear protrusion by decreasing the pressure on the disc or by placing tension on the posterior longitudinal ligament. Time of traction should be short in acute phase else there could be an increase in disc pressure leading to increased pain due to fluid imbibition ( less than 15 minutes of intermittent traction and less than 10 minutes of sustained traction).
Traction is contraindicated in disc protrussion medial to the nerve root.
c) EXERCISES FOR HERNIATED DISC- herniated disc exercises play a vital role in treatment of pain and inflammation. Extension exercises are useful in early treatment of disc related signs and symptoms.
Techniques to mechanically reduce a nuclear disc protrusion- These are used if the test movements show that these movements and postures improve the symptoms.
a) Posterior or posterolateral protrusion
i) Passive Extension- Patient is lying prone (i.e on belly). If patient is in such extreme pain, place pillows under the abdomen for support, gradually increase the amount of extension by removing pillows. Progress by having the patient prop himself up on the elbows, allowing the pelvis to sag. Wait for 5-10 minutes between each increment of extension to allow for reduction of water content and size of bulge. Progress by having patient prop on the hands. If sustained postures are not well tolerated, have the patient perform passive lumber extension intermittently by repeating the prone press ups.
ii) Lateral shift correction- If patient has lateral shift, first correct lateral shift then start with extension exercises. Therapist stands on the side to which the thorax is shifted and places his shoulder against the patient's elbow which is flexed against the rib cage. Therapist wraps the arms around patient's pelvis and pulls pelvis towards him while pushing the patient's thorax away.
Self correction: Patient places the hand on the side of the shifted rib cage on the lateral aspect of the rib cage and place the other hand over the crest of opposite ilium. Then gradually push these regions towards midline and hold.
b) Anterior protrusion
i) Correction of lateral shift- Patient stands in front of a chair and places the leg opposite to the shift on a chair so the hip is in about 90 degree of flexion. Leg on the side of lateral shift is kept extended. Patient then flexes the trunk onto the raised thigh and applies pressure by pulling on the ankle.
ii) Passive flexion- Bring both knees to the chest and hold this position with arm around the thighs.
c) Active range of motion exercises within painfree range to the lower limb can be done e.g ankle toe movements, heel drag, hip abduction/adduction.
d) Mobilization of thoracic spine Mobilization of segments above and below the affected segmental level.
e) Piriformis muscle stretching
f) Maintain/ improve mobility of neural tissues- These exercises should be performed with caution in acute stage, usually in recumbent position. These will prevent chronic complications from increased neural tension e.g passive SLR with foot dorsiflexion.
g) Hydrotherapy exercises
g) Patient education-These are some movements you should try to avoid:
* bending over to lift very heavy items
* performing squats with too much weight
* low back extensions, as they put high stress levels on discs
* running, since it can place strains on the discs
* any form of resistance training
SUB ACUTE STAGE:
Usually the acute symptoms decrease in 4-6 days.
a) Continue with the exercises done in acute phase e.g prone press ups, nerve mobility exercises, modalities.
b) Simple spinal movements in pain free ranges using gentle pelvic tilts. Pelvic rocking can be done in supine, sitting, prone lying, side lying, standing, quadripud (cat and camel exercise). Emphasize on anterior pelvic tilt so that spine is in extension. Pelvic rolling can be added.
c) Isometrics of extensors but caution against holding breath and causing valsalva.
d) Encourage aerobic activities, walking, swimming with patient's tolerance.
CHRONIC STAGE:
When the disc symptoms have stabilized.
Aims:
a) Restore range of motion.
b) Restore muscle strength, endurance and function.
c) Retrain kinesthetic awareness and control of normal alignment.
d) Patient involvement and education to manage posture to prevent recurrences.
PIVD Exercises In Chronic Stage
a) Gentle active painfree range of motion exercisesAfter 3 weeks from the onset of PIVD symptoms, start side flexion and extension in standing. Progress to adding flexion only when the disc has healed.
b) Stretching and flexibility exercises Stretching of the lumbar erector spinae and soft tissues posterior to the spine ( knee to chest position). Following any flexion exercises, conclude with extension exercises such as prone press ups/ standing back extension.
Hamstring stretch: Lie on your back with your knees bent. Raise one leg slowly and place your hands behind your knee. Straighten your leg as much as you can, and gently pull it toward your chest. Hold for a few seconds, then return to the starting position and repeat with the other leg. Do not force this exercise! You should feel a stretch in the back of your thigh. If you feel pain or discomfort anywhere else, discontinue this exercise until you are stronger.
c) Core stability exercises-Whenever there is a slight imbalance in the core muscles, you suffer from back pain. Core strengthening exercises help in relieving back pain and form the base of the core stability training program. The aim of these exercises is to provide more support to your back by strengthening the muscles of your spine.
- The Bridge: Strengthens several core muscle groups - e.g buttocks, back, abs for PIVD patients. Lie flat on back; bend knees at 90-degree angle, feet flat on floor. Tighten abs. Raise buttocks off floor, keeping abs tight. Tighten buttocks. Shoulder to knees should be in straight line. Hold for a count of five. Slowly lower buttocks to floor. Repeat five to fifteen times.
- The Plank: Strengthening exercise for back, abs and neck (also strengthens arms and legs)for PIVD patients. Lie on stomach, place elbows and forearms on floor. In a push-up position, balance on your toes and elbows. Keep your back straight and legs straight. (Like a plank) Tighten abs. Hold position for 10 seconds. Relax. Repeat five to ten times. If this exercise is too difficult (as it often is for beginners), balance on your knees instead of your toes.
The Side Plank: Strengthens the obliques (side abdominal muscles)for PIVD patients. Lie on right side. Place right elbow and forearm on floor. Tighten abs. Push up until shoulder is over elbow. Keep your body in a straight line – feet, knees, hips, shoulders, head aligned. Only forearm and side of right foot are on floor (feet are stacked). Hold position for 10 seconds. Relax. Repeat five times. Repeat on left side. If this exercise is too difficult, balance on stacked knees (bend knees and keep feet off floor) instead of feet.
The Wall Squat: Strengthening exercise for back, hips and quads in PIVD patients. Stand with your back against a wall, heels about 18 inches from the wall, feet shoulder-width apart. Tighten abs. Slide slowly down the wall into a crouch with knees bent to about 90 degrees. If this is too difficult, bend knees to 45 degrees and gradually build up from there. Count to five and slide back up the wall. Repeat 5 -10 times.- Leg and arm raises: Strengthening exercise for back and hip muscles in PIVD patients. Lie on stomach, arms reached out past your head with palms and forehead on floor. Tighten abs. Lift one arm (as you raise your head and shoulders) and the opposite leg at the same time, stretching them away from each other. Hold for 5 seconds and then switch sides. Repeat 5 - 10 times.
- Leg lifts: Quad Strengthening Exercise for PIVD patients. Lie flat on back. Bend left knee at 90-degree angle, keeping foot flat on floor. Tighten abs. Keep the right leg straight and slowly lift right foot to the height of the left knee. Hold for a count of 3. Do 10 repetitions. Switch sides and repeat.
Basic Crunches: upper abdominal exercise for PIVD patients.
Lie on back, knees bent, feet flat on floor. Do not anchor feet. (Anchoring the feet or keeping the legs straight along the floor can strain the lower back). Head and back should be in neutral position. A rolled up towel may be placed under the natural curve of the lower back to provide extra support - the small of the back should be about an inch above the floor. Place hands behind head with elbows pointing outward. Your hands are used to support your head (to avoid neck from tiring out before abs) but do not pull head forward.Tighten abs. Raise your head and shoulders off the floor - three to six inches is enough. Look at the ceiling to help prevent tilting your head. Keep elbows back.Exhale when raising your torso off the floor and inhale when lowering. Do ten - fifteen repetitions.
d)Strengthening exercises-
*Opposite Arm and Leg Extension: balancing / stabilization exercise for PIVD patients: Strengthens muscles running down sides of spine, back of shoulders, hips and buttocks. Begin on all fours, hands directly under your shoulders and knees directly under your hips. Keep head aligned with spine (to help avoid tilting head, look at floor). Keep buttocks and abdomen tight. Do not arch the back. Lift one arm up and forward until it is level with torso; simultaneously lift the opposite leg in the same manner. Keep arm, spine, and opposite leg aligned as if they are forming a tabletop. Balance yourself for 10 seconds then slowly return to starting position. Switch sides and repeat. Remember to breathe. Do five repetitions.
*Leg Lifts: lower abdominal exercise for PIVD patients. Lie flat on back. Bend left knee at 90-degree angle, keeping foot flat on floor. Tighten abs. Keep the right leg straight and slowly lift it until right foot is at the height of the left knee. Hold for a count of 5. Do 5 to 15 repetitions. Switch sides and repeat.
*Backward Leg Swing: Gluteal exercise for PIVD patients.
(The muscles of the buttocks help support the spine) Stand, holding onto the back of a chair for support. Tighten abs. Swing leg back at a diagonal until you feel your buttocks tighten. Tense muscles as much as you can and swing leg back a couple more inches. Return leg to floor. Do 10 - 15 repetitions. Switch sides and repeat.
*Abdominal strengthening exercises: Isometric abs, knee to chest, bicycle exercises.
e) Hydrotherapy exercises for back pain-
- Warm up, mobilising exercises
- Stretching exercises
- Strengthening exercises
- Relaxatation exercises
- Swimming workouts
Read research articles about PIVD on PubMed
Patient Education:
*Teach safe movement patterns and body mechanics.
*Teach patient preventive exercises and mechanics for relief of mechanical stress in daily activities.
*Teach relaxation exercises to cope with muscle tension.
*Instruct patient on how to modify environment e.g bed, chairs, car seats, work area etc.
Return from PIVD to Orthopedic Physiotherapy
Recent Articles
|
Author's Pick
Rating: 4.4 Votes: 252 |

