Enhance your health with free online physiotherapy exercise lessons and videos about various disease and health condition
Tendinosis vs Tendinitis
Tendinosis is intratendinous atrophy and degeneration with a relative absence of inflammation; a palpable nodule may be present over tendon.
Tendinitis is symptomatic degeneration of the tendon with vascular disruption and inflammatory repair response.
Comparison of Overuse Tendinosis and Overuse Tendinitis
Comparison Factors
Tendinosis
Tendinitis
Prevalence
Common
Uncommon
Time for full recovery (initial)
2-3 months
2-3 days
Time for full recovery (chronic)
3-6 months
4-6 wk
Likelihood of full recovery
About 80%
99%
Focus of conservative therapy
Encourage collagen synthesis, maturation, and strength
Anti-inflammatory therapy and drugs
Role of surgery
Excise abnormal tissue
Not known
Prognosis of surgery
70% to 85%
95%
Surgical recovery
4-6 month
3-4 wk
TENDINOPATHIES
Tendinopathy is a clinical condition characterized by activity-related pain, focal tendon tenderness, and intratendinous imaging changes. It represents a common and significant problem, with a prevalence of 14% in elite athletes, and requires a recovery time of 3 to 6 months with first-line conservative management. Historically, it was thought to be one of inflammation, and consequently, the condition was labeled tendinitis. However, recent histopathologic studies have shown the underlying pathology to be primarily one of tendon degeneration (tendinosis)
Although the pathologic label tendinosis has been in use for more than 25 years to describe collagen degeneration in tendinopathy, many clinicians still use the term tendinitis to describe painful chronic overuse injury, implying that the fundamental problem is inflammatory. Maffulli and colleagues advocate the use of the term tendinopathy as a generic descriptor of clinical conditions such as pain, swelling, and impaired performance in and around tendons arising from overuse, with the labels tendinosis and tendinitis most appropriately applied after histopathologic examination. This nomenclature separates chronic degeneration of tendons from acute and mainly inflammatory processes, with implications for treatment and management (Table).
Common Tendinopathies
- Rotator Cuff Tendinopathies
- Lateral Epicondylitis/Tennis Elbow
- Medial Epicondylitis/Golfer's Elbow
- De Quervain’s Syndrome
- Extensor Carpi Ulnaris Tendinitis
- Patellar Tendinopathy
- Achilles Tendon Disorders
Based on the anatomical location of the histopathological changes, it is possible to classify microtraumatic tendon injury into four types (1) tendinitis - tendon strain or tear; (2) tendinosis- intratendinous degeneration; (3) paratenonitis - inflammation of the paratenon only; and (4) paratenonitis with tendinosis.
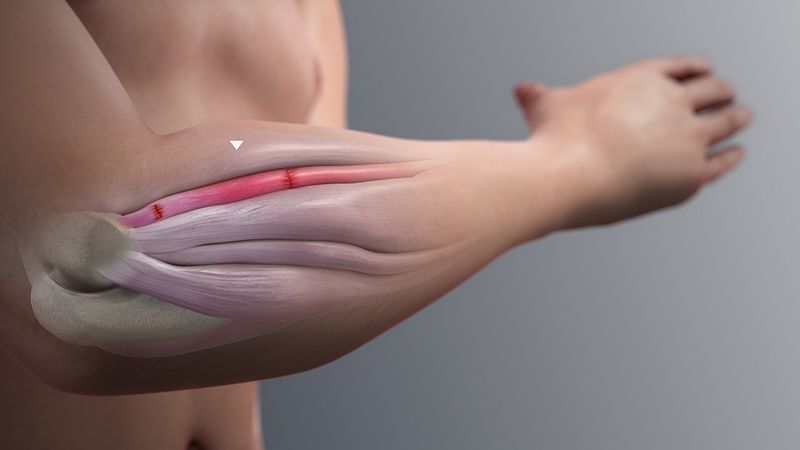 Author www.scientificanimations.com
Author www.scientificanimations.comClassification of Tendon Disorders
New
Old
Definition
Histologic Findings
Clinical Signs & Symptoms
Paratenonitis
Tenosynovitis Tenovaginitis Peritendinitis
Inflammation of only the paratenon whether or not lined by synovium
Inflammatory cells in paratenon or peritendinous areolar tissue
Cardinal inflammatory signs: warmth, swelling, pain, crepitation, local tenderness, dysfunction
Paratenonitis with tendinosis
Tendinitis
Paratenon inflammation associated with intratendinous degeneration
Same as above, with loss of tendon, collagen fiber disorientation, scattered vascular ingrowth, but no prominent intratendinous inflammation
Same as above, often with palpable tendon nodule, swelling, and inflammatory signs
Tendinosis
Tendinitis
Intratendinous degeneration due to atrophy (aging, microtrauma, vascular compromise)
Noninflammatory intratendinous collagen degeneration with fiber disorientation, hypocellularity, scattered vascular ingrowth, occasional local necrosis, or calcification
Often palpable tendon nodule that may be asymptomatic but may also be point tender; swelling of tendon sheath is absent.
Tendinitis
Tendon strain or tear
Symptomatic overload of the tendon with vascular disruption and inflammatory repair response
Three recognized subgroups: each displays variable histologic characteristics from purely inflammation with acute hemorrhage and tear to inflammation superimposed on preexisting degeneration, to calcification and tendinosis changes in chronic conditions. In the chronic stage, it may be
- interstitial microinjury,
- central tendon necrosis,
- frank partial rupture, or
- acute complete rupture
Symptoms are inflammatory and proportional to vascular disruption, hematoma, or atrophy-related cell necrosis.
Symptom duration defines each subgroup:
- A: Acute (<2 wk)
- B: Subacute (4-6 wk)
- C: Chronic (>6 wk)
Treating Tendon Injury
General Principles
The basic principles governing clinical intervention during tendon healing are outlined in Table 3. The initial clinical assessment of the patient must include a thorough history and physical examination, identifying, in particular, any intrinsic or extrinsic factors that may be contributing to the tendon injury. The exact anatomical site of the disease is located, and an estimate of the stage of healing should be made based on the degree of pain and inflammation. Imaging techniques, such as ultrasound and MRI, may be of help in this process. Establishing the stage of healing will determine the appropriate focus for initial treatment. In general, the treatment protocol should include:
- the correction of existing intrinsic and extrinsic etiological factors;
- control of pain and inflammation, using drugs, ice, and other modalities; and
- instituting early motion, beginning with passive movement and stretching, then progressing to active exercises.
Principles governing clinical intervention during stages of tendon healing
Inflammatory
Fibroblastic/proliferation
Remodeling/Maturation
Time (days)
0-6
5-21
20 days and onwards
Suggested therapy
Rest, ice, anti-inflammatory modaLities, decreased tension
Gradual introduction of stress. modalities to increase collagen syntheses
Progressive stress on tissue
Physiological rationale
Prevent prolonged inflammalion, prevent disruption of new blood vessels and collagen fibrils, promote ground substance syntheses
lncrease collagen, increase collagen cross-Iinking, increase fibril size and alignment
Increase cross-Iinking (tendons and ligaments), decrease crosslinking( joint capsule), increase fibril size
Main aims
Avoid new tissue disruption
Prevent excessive muscle and joint atrophy
Optimise tissue healing
Physical Therapy Treatment and self-care recommendations for tendinosis include:
- Rest.
- Adjust ergonomics and biomechanics.
- Use appropriate support. Physical therapists can also recommend appropriate support to reduce tensile stress on the tendon, such as bracing or taping
- Stretch and keep moving, though conservatively
- Apply ice. Use ice for 15–20 minutes several times a day (allowing for at least 45 minutes in between icing session), and after engaging in activities that utilize the tendon
- Eccentric strengthening. An eccentric strengthening regimen done 1–2 times daily for 12 weeks has been clinically proven to be a very successful treatment for tendinopathis, especially when the exercises are performed slowly. Eccentric strengthening is “lengthening a muscle while it is loaded and contracting.
- Massage. Massage stimulates circulation and cell activity, especially when done at the appropriate depth. Deep-friction massage applied to the tendon serves to stimulate fibroblast activity and generate new collagen.
- Nutrition. Vitamin C, manganese, and zinc are all important for the synthesis of collagen production. Vitamin B6 and Vitamin E have also been linked to tendon health.
References
- Maffulli N, Khan KM, Puddu G: Overuse tendon conditions: time to change a confusing terminology. Arthroscopy 14:840–843, 1998.
- Clancy WGJ: Tendon trauma and overuse injuries. In Leadbetter WB, Buckwalter JA, Gordon SL (eds): Sports-Induced Inflammation: Clinical and Basic Science Concepts. Park Ridge, Ill, American Academy of Orthopaedic Surgeons, 1990, pp 609-618.
- Khan K, Cook J: The painful nonruptured tendon: Clinical aspects. Clin Sports Med 22:715, 2003
- Curwin SL (1998) The aetiology and treatment of tendinitis. In: Harries M, Williams C, Stanish WD, Micheli LJ (eds) Oxford textbook of sports medieine. Oxford, UK, Oxford University Press, pp 610-630
- Tendinopathy- NCBI
Back to Sports Physical Therapy
Back to Home Page
Recent Articles
|
Author's Pick
Rating: 4.4 Votes: 252 |

