Enhance your health with free online physiotherapy exercise lessons and videos about various disease and health condition
Total Knee Replacement Rehabilitation
Total Knee Replacement Rehabilitation aims at preventing hazards of bedrest, assist with adequate functional ROM and strengthening knee musculature to obtain independent activities of daily living.
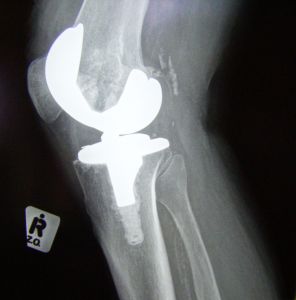
A total knee replacement (TKR) is usually done as the surgical treatment option for advanced osteoarthritis of the knee joint.During the surgery, the knee joint is replaced with artificial material. The knee joint is made up of the femur (thigh bone), the tibia (shin bone), the patella (knee cap) and cartilage (usually worn out because of OA).The end of the femur is removed and replaced with a metal surface and the top of the tibia is removed and replaced with a plastic piece that has a metal stem. If the knee cap has also degenerated, a plastic piece may be added to the back surface to create a smoother joint surface.
Indications for Total Knee Arthoplasty
- disabling knee pain with functional impairment
- radiographic evidence of significant arthritic involvement
- failed conservative measures including ambulatory aids (canes), NSAIDS, and lifestyle modification.
Contraindications for Total Knee Replacement
Absolute
- joint infection
- sepsis or systemic infection
- neuropathic arthropathy
- painful solid knee fusion (usually due to RSD. RSD is not helped by additional surgery)
Relative
- severe osteoporosis
- debilitated poor health
- nonfunctioning extensor mechanism
- significant peripheral vascular disease
Goals Of Total Knee Replacement Rehabilitation
- Prevent hazards of bedrest like DVT, pulmonary embolism, pressure ulcers.
- Assist with adequate and functional range of motion.
- Strengthen the knee musculature.
- Assist patient in achieving functional independent activities of daily living.
- Independent ambulation with an assistive device.
Perioperative considerations for Total Knee Replacement Rehabilitation
Component design, fixation method, operative technique (osteotomy, extensor mechanism technique), bone quality will all affect perioperative rehabilitation. Implant can be posterior cruciate ligament (PCL) retaining, PCL sacrificing, or PCL sacrificing with substitution.
Rehabilitation of Patients with Hybrid Ingrowth Implant versus those with Cemented knee Implant
Cemented Total Knee Arthroplasty
Ability for weight bearing as tolerated (WBAT) with walker from 1 day postoperative.
Hybrid or Ingrowth Total Knee Arthroplasty
Touch down weight bearing (TDWB) only with walker for first 6 weeks. Next 6 weeks, begin crutch walking with weight bearing as tolerated. Surgeon's preferences may be different.
Total Knee Replacement Rehabilitation Outline
Preoperative Physical Therapy
- Review bed to chair transfers, bathroom transfers, tub transfers with tub chair at home.
- Teach postoperative knee exercises and give patient handout.
- Teach ambulation with assistive devices TDWB or WBAT at the discretion of the surgeon.
- Review precautions.
Inpatient Total Knee Replacement Rehabilitation Goals
- 0-90 degree ROM in the first 2 weeks before discharge from an inpatient setting.
- Rapid return of quadriceps control and strength to enable patient to ambulate without knee immobiliser.
- Rapid mobilisation to minimize risk of bedrest.
Day 1
FOLLOW THE VIDEOS FOR BETTER UNDERSTANDING OF THE EXERCISES IN Total Knee Replacement Rehabilitation
- Ankle pump
- Initiate isometric exercises.
- Quads sets Lie on your back with legs straight, together, and flat on the bed, arms by your side. Perform this exercise one leg at a time. Tighten the muscles on the top of one of your thighs. At the same time, push the back of your knee downward into the bed. The result should be straightening of your leg. Hold for 5 seconds, relax 5 seconds; repeat 10 times for each leg.
- SLR This exercise helps strengthen the quadriceps muscle also. Bend the uninvolved leg by raising the knee and keeping the foot flat on the bed. Keeping your involved leg straight, raise the straight leg about 6 to 10 inches. Hold for 5 seconds. Lower the leg slowly to the bed and repeat 10-20 times.
Once you can do 20 repetitions without any problems, you can add resistance (ie. sand bags) at the ankle to further strengthen the muscles. The amount of weight is increased in one pound increments.
- Ambulate twice a day with knee immobilizer, assistance, and walker.
- Cemented prosthesis: Weight bearing as tolerated (WBAT) with walker.
- Noncemented prosthesis: TDWB with walker.
- Transfer out of bed and into the chair twice a day with leg in full extension on stool or another chair.
- CPM machine- Do not allow more than 40 degrees of flexion on settings until after 3 days. Usually 1 cycle per minute. Progress 5-10 degrees a day as tolerated.
- Initiate active ROM and active assisted ROM exercises.
- During sleep place a pillow under the ankle to help passive knee extension.
Ice: Ice may be used during your hospital stay and at home to help reduce the pain and swelling in your knee. Pain and swelling will slow your progress with your exercises. A bag of crushed ice may be placed in a towel over your knee for 15-20 minutes. Your sensation may be decreased after surgery, so use extra care.
Day 2-2 weeks
- Continue isometric exercises throughout Total Knee Replacement Rehabilitation.
- Perform vastus medialis oblique (VMO) strengthening by terminal knee extension-Lie on your back with a blanket roll under your involved knee so that the knee bends about 30-40 degrees. Tighten your quadriceps and straighten your knee by lifting your heel off the bed. Hold 5 seconds, then slowly your heel to the bed. You may repeat 10-20 times.
- Begin gentle passive ROM exercises for knee- knee extension, knee flexion, heel slides, wall slides.
- Begin patellar mobilization techniques when incision stable to avoid contracture.
- Perform active hip abduction and adduction exercises.
- Continue active and active assisted knee ROM exercises.
- Continue and progress these exercises until 6 weeks after surgery. Give home exercises with outpatient physical therapist following patient 2-3 times per week.
- Plan discharge when ROM of involved knee is from 0-90 degrees and patient can independently execute transfers and ambulation.
2-3 weeks
- Continue previous exercises.
- Continue walking with walker until otherwise instructed by surgeon.
- Prescribe prophylactic antibiotics for possible eventual dental or urological procedures.
- Driving is not allowed for 4-6 weeks.
- Orient family to patient's needs, abilities, and limitations.
Review tub transfers in Total Knee Replacement Rehabilitation
- Many patients lack sufficient strength, ROM, or agility to step over tub for showering.
- Place tub chair as far back in tub as possible, facing the faucets. Patient backs up to the tub, sits on the chair, and then lifts the leg over.
- Tub mats and nonslip stickers for tub floor traction also are recommended.
6 weeks onwards in Total Knee Replacement Rehabilitation
- Begin weight bearing as tolerated with ambulatory aid, if this has not already begun.
- Perform wall slides and lunges.
- Perform step ups.
- Begin closed chain knee exercises on total gym and progress over 4-5 weeks for bilateral lower extremities.
- Perform cone walking with progression.
- Progress to stationary bicycling.
Know more about Knee Replacement Here- Knee Replacement Wiki Resource
Other Considerations For the next 4-6 weeks after surgery
- Avoid sexual intercourse. Sexual activity can usually be resumed after your 6-week follow-up appointment.
- You can usually return to work within two to three months, or as instructed by your doctor.
- You should not drive a car until after the 6-week follow-up appointment.
- Continue to wear elastic stockings (TEDS) until your return appointment.
- No shower or tub bath until after staples are removed.
- When using heat or ice, remember not to get your incision wet before your staples are removed.
Return from Total Knee Replacement Rehabilitation to Orthopedic Physiotherapy
Return from Total Knee Replacement Rehabilitation to Home Page
Recent Articles
|
Author's Pick
Rating: 4.4 Votes: 252 |

