Enhance your health with free online physiotherapy exercise lessons and videos about various disease and health condition
Legg Calve Perthes disease
legg calve perthes disease
Idiopathic osteonecrosis of the femoral head in a skeletally immature patient, is characterized by necrosis of the ossific nucleus of the femoral head secondary to occlusion of the arterial or venous blood supply. After infarction, healing occurs by creeping substitution and resorption of the dead bone. The resulting deformity of the hip joint may be extensive and can exceed the remodeling and healing capacity of the developing epiphysis.
Signs & Symptoms of Legg Calve Perthes disease
Patients with Legg Calve Perthes disease present with pain in the groin, thigh, or knee region. Onset usually is insidious, and the patient may be symptomatic before presentation. Most children have a Trendelenburg gait. Internal rotation, abduction, and extension of the hip are limited.
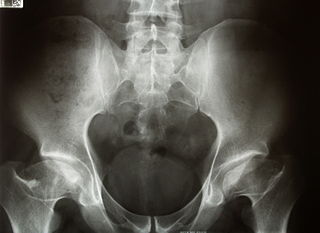
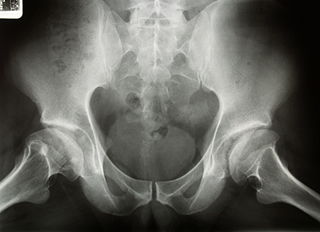
Diagnosis
Plain radiographs are essential for diagnosis and can be predictive of outcome. Several classification systems have been proposed, including the Caterall, Herring, Salter, and Waldenstrom systems. All these classification systems used different graduated radiologic criteria to assist in predicting outcome. “Head at risk” signs have also been proposed to help predict outcome and include Gage’s sign (a radiolucent wedge defect on the lateral side of the epiphysis), calcification lateral to the epiphysis, lateral subluxation of the femoral head, a horizontal physis, and metaphyseal cysts.
Treatment for Perthes Disease
Nonoperative
Treatment is based on containment of the avascular femoral head within the acetabulum to allow healing and remodeling of the affected cartilage. Restricted activity and limited weight-bearing can help control the symptoms and prevent further deformation of the femoral head. The most important factor for healing is age and amount of femoral head involvement; younger patients with little deformity have a better chance of normal cartilage development. During the treatment period, it is essential that range of motion of the hip is preserved and aggressive physical therapy is warranted. Treatment is continued until plain radiography shows reossification of the ossific nucleus and lateral coverage for the femoral head, and the patient is symptom free. Long-term risks in athletes with Legg Calve Perthes disease include the risk for early arthritis secondary to the amount of residual femoral head collapse. Patients are prone to overuse syndromes because of joint incongruity.
Physiotherapy Interventions
Physiotherapy interventions have been shown to improve ROM and strength in this patient population. Patients demonstrate greater improvement in muscle strength, functional mobility, gait speed, and quality of exercise performance.
Physiotherapy Goals
- Reduce pain
- Increase ROM
- Increase strength
- Patient to be independent with the appropriate assistive device and weight bearing precautions
- Improve balance
- Improved efficiency in walking
Physiotherapy Treatment Interventions for
Pain
ROM (range of motion)
- Static stretch for Lower Extrimity musculature with or without use of a hot pack
- Dynamic ROM and active assistive range of motion (AAROM) may be appropriate if the patient is muscle guarding due to pain
- Perform AROM and AAROM following passive stretching to maintain newly gained ROM
- Perform stretching in a position that is suitable for the individual and include hip Internal Rotation, hip External Rotation, hip abduction, hip extension, and any other lower extremity motion that is significantly limited
Strength
- Begin with isometric exercise and progress to isotonic exercises in a gravity lessened position with further progression to isotonic exercises against gravity. Include concentric and eccentric contractions
- Focus on strengthening of hip abductors, hip flexors, hip external rotators, hip internal rotators, hip extensors, or any other lower extremity muscle group that displays significant strength deficits. Special attention is to be given to the gluteus medius in order to minimize intraarticular pain and for pelvic control during single leg activities and ambulation.
- Performance of weight bearing vs. non-weight bearing exercises is based on the weight bearing status as determined by the physician, patient’s tolerance to weight bearing positions, and safety
- Closed chain double limb exercises with light resistance (less than full body weight) may be performed
- It is not recommended to perform single limb closed chain exercises on the involved side due to increased intra-articular pressure in the hip joint
Balance
- Activities that include double limb stance and a narrowed base of support on stable surfaces may be performed if weight bearing status and symptoms allow
- It is not recommended to perform single limb activities due to increased intra-articular pressure in the hip joint
Gait
- Follow the referring physician’s guidelines for weight bearing status.
- Begin gait training with the appropriate assistive device given weight bearing status as determined by the referring physician or based on the patient’s tolerance to full weight bearing due to pain or safety.
Operative
Surgical treatment during the acute disease can help to control symptoms and to contain the hip. Hip arthroscopy has been shown to be therapeutic for patients with Legg Calve Perthes disease. Removal of loose bodies and debridement of cartilage flaps provide most of the therapeutic benefit. Other operations include a wide spectrum of femoral osteotomies, acetabular osteotomies, and shelf procedures, with the goal of providing containment for the femoral head.
Return from legg calve perthes disease to Orthopedic Physical Therapy
Return from legg calve perthes disease to Home Page
Reference
- Legg–Calvé–Perthes syndrome. From Wikipedia, the free encyclopedia
- Legg-Calve-Perthes disease. Mayoclinic
- Kim HK. Legg-Calvé-Perthes disease. J Am Acad Orthop Surg. 2010 Nov;18(11):676-86.
- Manfred Nelitz, Dr. med., Sabine Lippacher, Dr. med., Rüdiger Krauspe.Perthes Disease-Current Principles of Diagnosis and Treatment. Dtsch Arztebl Int. Jul 2009; 106(31-32): 517–523.
Recent Articles
|
Author's Pick
Rating: 4.4 Votes: 252 |

