Enhance your health with free online physiotherapy exercise lessons and videos about various disease and health condition
Managing Fibromyalgia an urban ache
Comprehensive approach to Managing Fibromyalgia
What is Fibromyalgia?
Fibromyalgia (FMS) refers to a condition with a constellation of symptoms that include widespread aching, stiffness, fatigue, and the presence of specific body tender points. The presence of pain originates in the muscles and connective tissues of the body. It is a syndrome of unknown aetiology characterized by chronic wide spread pain, increased tenderness to palpation and additional symptoms such as disturbed sleep, stiffness, fatigue and psychological distress. While medication mainly focus on pain reduction, physical therapy is aimed at managing fibromyalgia consequences such as pain, fatigue, deconditioning, muscle weakness and sleep disturbances and other disease consequences. Connective tissues contain fibrocytes, or fibre cells, muscles contain myocytes, or muscle cells, and together with the Latin word for pain, “algia,” the word fibromyalgia is constructed. The exact physiological process has not been determined, but it is likely many factors, including those beyond the muscles and fibrous tissues, play a role.
Since many patients with joint and ligament pain have been referred to rheumatologists, to check whether inflammation is present that would respond to anti-inflammatory drugs, this medical specialty developed criteria for the diagnosis of this illness.
The American College of Rheumatologists (ACR) defined fibromyalgia (FMS) in 1990 as the presence of-
- 1) body or joint pain above and below the waist, and on the right and left side of the body,
- 2) axial pain (most often neck or low back pain), and
- 3) 11 out of 18 possible tender points.
Patients most often have associated fatigue, sleep disorders, irritable bowel syndrome, migraine headaches, immune system or endocrine system disorders. When the joints and ligaments are examined by clinicians, there is surprisingly little inflammation present for the amount of pain that is experienced. In fact, muscle and ligament examinations from biopsy samples characteristically show no unusual patterns of disease or inflammation. About 2-5% of the general population is considered to have FMS. FMS is a common disorder characterized by multiple tender points, widespread deep muscle pain, fatigue, and depression.
What are tender points?
Tender points are pain points or localized areas of tenderness around joints, but not the joints themselves. These tender points hurt when pressed with a finger. Tender points are often not deep areas of pain. Instead, they are superficial areas seemingly under the surface of the skin, such as the area over the elbow or shoulder.
How many tender points are important for FMS?
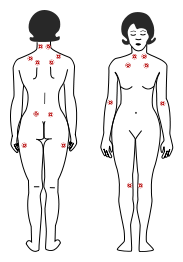
There are 18 tender points important for the diagnosis of fibromyalgia (see picture below). These tender point are located at various places on your body. To get a medical diagnosis of FMS, 11 of 18 tender point sites must be painful when pressed. In addition, for a diagnosis of fibromyalgia, the symptom of widespread pain must have been present for three months.
FMS trigger points exist at these nine bilateral muscle locations:
- Low cervical region: (front neck area) at anterior aspect of the interspaces between the transverse processes of C5-C7.
- Second rib: (front chest area) at second costochondral junctions.
- Occiput: (back of the neck) at suboccipital muscle insertions.
- Trapezius muscle: (back shoulder area) at midpoint of the upper border.
- Supraspinatus muscle: (shoulder blade area) above the medial border of the scapular spine.
- Lateral epicondyle: (elbow area) 2 cm distal to the lateral epicondyle.
- Gluteal: (rear end) at upper outer quadrant of the buttocks.
- Greater trochanter: (rear hip) posterior to the greater trochanteric prominence.
- Knee: (knee area) at the medial fat pad proximal to the joint line.
Is there a prescription medication that help managing fibromyalgia pain?
Managing Fibromyalgia Pain for tender points with involves a multifaceted treatment program that employs both conventional and alternative therapies. While the reason is not entirely clear, FMS pain and fatigue sometimes respond to low doses of antidepressants. However, the standard treatment for managing fibromyalgia (Chronic fatigue syndrome) and tender points involves medications, daily stress management, exercise, physiotherapy, hydrotherapy using heat and ice, and rest. Other remedies for symptoms may also be used in managing fibromyalgia.
What at-home treatments might help in managing fibromyalgia tender point pain?
Alternative treatments or home remedies are important in managing fibromyalgia and the pain of tender points. As an example, therapeutic massage can manipulate the muscles and soft tissues of the body to help ease pain, muscle tension, spasms, and stress.
Twice daily moist heat applications are also helpful in easing the deep muscle pain and stiffness. To benefit from moist heat, you can use a moist heating pad, warm shower, or a heat "cozy" that you warm in the microwave.
With chronic fatigue syndrome, it's extremely important to manage your schedule and to control your level of stress. Be sure to block time each day to rest and relax. Avoid making too many commitments that can increase stress and fatigue. In addition, you can do relaxation exercises such as guided imagery, deep-breathing exercises, or the relaxation response to manage how you respond to stress.
Staying on a regular bedtime routine is also important. Doing so allows your body to rest and repair itself. In addition, regular exercise is vital to managing fibromyalgia pain, depression, and other symptoms of fibromyalgia.
A number of factors can make FMS symptoms worse. They include:
- Anxiety
- Changes in weather -- for example, cold or humidity
- Depression
- Fatigue
- Hormonal fluctuations such as PMS or menopause
- Infections
- Lack of sleep or restless sleep
- Periods of emotional stress
- Physical exhaustion
- Sedentary lifestyle
What Are the Symptoms of Fibromyalgia?
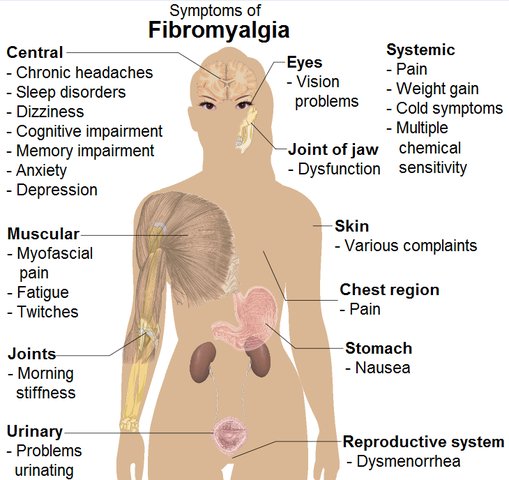
Symptoms of FMS include:
- Chronic muscle pain, muscle spasms or tightness, and leg cramps
- Moderate or severe fatigue and decreased energy
- Insomnia or waking up feeling just as tired as when you went to sleep
- Stiffness upon waking or after staying in one position for too long
- Difficulty remembering, concentrating, and performing simple mental tasks
- Abdominal pain, bloating, nausea, and constipation alternating with diarrhoea (irritable bowel syndrome)
- Tension or migraine headaches
- Jaw and facial tenderness
- Sensitivity to one or more of the following: odours, noise, bright lights, medications, certain foods, and cold
- Feeling anxious or depressed
- Numbness or tingling in the face, arms, hands, legs, or feet
- Increase in urinary urgency or frequency (irritable bladder)
- Reduced tolerance for exercise and muscle pain after exercise
- A feeling of swelling (without actual swelling) in the hands and feet
- Painful menstrual periods
- Dizziness
FMS symptoms may intensify depending on the time of day -- morning, late afternoon, and evening tend to be the worst times, while 11 a.m. to 3 p.m. tends to be the best time. They may also get worse with fatigue, tension, inactivity, changes in the weather, cold or drafty conditions, overexertion, hormonal fluctuations (such as just before your period or during menopause), stress, depression, or other emotional factors.
If the condition is not diagnosed and treated early, symptoms can go on indefinitely, or they may disappear for months and then recur.
What causes fibromyalgia?
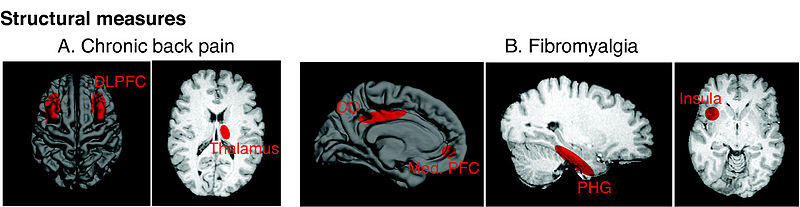
The exact cause is not known. Patients experience pain in response to stimuli that are normally not perceived as painful. Researchers have found elevated levels of a nerve chemical signal, called substance P, and nerve growth factor in the spinal fluid of fibromyalgia patients. The brain nerve chemical serotonin is also relatively low in patients with chronic fatigue syndrome. Studies of pain in fibromyalgia have suggested that the central nervous system (brain) may be somehow supersensitive. Scientists note that there seems to be a diffuse disturbance of pain perception in patients with FMS.
Other researchers believe fibromyalgia is caused by a lack of deep sleep. It is during stage 4 sleep that muscles recover from the prior day's activity, and the body refreshes itself. Sleep studies show that as people with FMS enter stage 4 sleep, they become more aroused and stay in a lighter form of sleep. Even though they may sleep for a long period of time, they get poor quality sleep. Also, patients with fibromyalgia have impaired non-Rapid-Eye-Movement, or non-REM, sleep phase (which likely explains the common feature of waking up fatigued and un refreshed in these patients). The onset of FMS has been associated with psychological distress, trauma, and infection.
Doctors don't know what causes fibromyalgia, but it most likely involves a variety of factors working together. These may include:
- Genetics. Because FMS tends to run in families, there may be certain genetic mutations that may make you more susceptible to developing the disorder.
- Infections. Some illnesses appear to trigger or aggravate FMS.
- Physical or emotional trauma. Post-traumatic stress disorder has been linked to FMS.
- Stress-induced pathophysiology
- Consequence of sleep disturbance
- Central dopamine dysfunction (hypodopaminergia)
- Deficient human growth hormone (HGH) secretion
- Other hypotheses-Other hypotheses have been proposed related to various toxins from the patient's environment, viral causes such as the Epstein-Barr Virus, an aberrant immune response to intestinal bacteria, and erosion of the protective chemical coating around sensory nerves. Still another hypothesis regarding the cause of fibromyalgia symptoms proposes that affected individuals suffer from vasomotor dysregulation resulting in sluggish or improper vascular flow.
Diagnosis
Fibromyalgia is considered a controversial diagnosis, with some authors contending that the disorder is a ‘non-disease’, due in part to a lack of abnormalities on physical examination, objective laboratory tests or medical imaging studies to confirm the diagnosis. While historically considered either a musculoskeletal disease or neuropsychiatric condition, evidence from research conducted in the last three decades has revealed abnormalities within the central nervous system affecting brain regions that may be linked both to clinical symptoms and research phenomena. Although there is as yet no generally accepted cure for fibromyalgia, there are treatments that have been demonstrated by controlled clinical trials to be effective in managing fibromyalgia symptoms, including medications, patient education, exercise, and behavioural interventions.
Diagnostic Criteria
The difficulty with diagnosing FMS lies in the fact that, in most cases, laboratory testing appears normal and that many of the symptoms mimic those of other disorders. A definite diagnosis of fibromyalgia syndrome should only be made when no other medical disease can explain the symptoms. This is to say, FMS is a diagnosis of exclusion.
A proper history and physical exam coupled with blood work and/or x-rays may be done to rule out:
- Hormonal imbalance
- Anaemia
- Infection
- Muscle disease
- Bone disease
- Nerve disease
- Joint disease
- Cancer
- Rheumatoid arthritis
- Hypothyroidism (including primary hypothyroidism, secondary hypothyroidism, Hashimoto’s thyroiditis, iodine deficiency goiter, and genetic thyroid enzyme defects). Thyroid-stimulating hormone levels should be checked routinely because this condition can mimic many of the symptoms of Chronic fatigue syndrome
- Polymyalgia rheumatica
Electrical nerve and muscle testing, known as electromyography (EMG) or nerve conduction velocity (NCV), may also be done to check the muscles and nerves.
Discussion
Although the pathophysiology of fibromyalgia is unknown it is a very real syndrome. Treatment may provide only partial symptomatic relief. True FMS is a chronic condition requiring long term effort in managing fibromyalgia that may include physical therapy, exercise, patient education and reassurance along with sleep-enhancing medications like low dose tricyclic antidepressants.
Emergency physicians often see trigger points associated with simple self-limiting regional myofascial pain syndromes which appear to arise from muscles, muscle-tendon junctions, or tendon-bone junctions. Myofascial disease can result in severe pain, but typically in a limited distribution and without the systemic feature of fatigue. When symptoms recur or persist after the basic therapy above, or are accompanied by generalized complaints, refer the patient to a rheumatologist or primary care physician.
When the quadratus lumborum muscle is involved there is often confusion as to whether or not the patient has a renal, abdominal, or pulmonary ailment. The reason for this is the muscle's proximity to the flank and abdomen as well as its attachment to the 12th rib, which when tender, can create pleuritic symptoms. A careful physical exam, with palpation, active contraction, and passive stretching of this muscle reproducing symptoms, can save this patient from a multitude of laboratory and x ray studies.
Fibromyalgia Diet
No Specific Foods Improve FMS.
Although some patients report that the symptoms of FMS - like several other musculoskeletal disorders such as arthritis - can be alleviated by dietary measures, there is no specific diet plan for managing fibromyalgia. Comparatively few diet studies have been undertaken to assess the impact of food on managing fibromyalgia, and there is no clear evidence indicating that any specific foods help in managing fibromyalgia. Also, there is no clear medical evidence that dietary supplements improve symptoms. Indeed, blood and hair tests have revealed no pattern of mineral deficiency in chronic fatigue syndrome patients. Thus it is misleading to say there is an effective diet in managing fibromyalgia symptoms. Truth is, most dietary recommendations for this musculoskeletal disorder are based on incomplete evidence from patients who experience benefits when following certain eating plans. As a result, most dietary guidelines for managing fibromyalgia are based on general principles of healthy eating, and avoiding foods known to cause problems like high blood sugar (hyperglycaemia), food allergies, headaches, digestive disorders and fatigue.
While there is no specific diet for all fibromyalgia cases, different symptoms may suggest ways of improving your health through diet. As FMS sufferers often have one condition amplifying another (or several others), relieving even one can increase your quality of life, sometimes substantially.
A common thread in managing fibromyalgia seems to be a tendency to feel better when refined sugar, caffeine, alcohol, fried foods, red meat, and highly processed foods, are kept to a sound personal minimum in the diet. Many people benefit from cutting out all sugar for a month, which can severely reduce the craving for sweets, and allow your body to better manage its sugar intake when you add it back in. Sharply reducing your intake of caffeine in all forms, and fried, processed fatty foods, can improve cravings for these items in the same way and allow you to see if they are contributing to your health problems. Even if you do not have severe food triggers, eating a healthier diet can have long-term benefits for managing fibromyalgia. Try supplementing your current diet with greater quantities of raw or lightly cooked fruits and vegetables. Try substituting meats that are high in fat with fish or lean poultry. Drink plenty of water and take a good vitamin supplement to be sure that you are getting proper nutrition.
The 12 items to avoid are:
1. High fat dairy foods
2. White sugar and white flour
3. Fried foods
4. Preservatives, junk food, and salt
5. Red meat (especially salt cured, cured bacon, smoked, or nitrate cured)
6. Coffee and caffeinated teas
7. Colas, soda pop, and carbonated beverages
8. Liquid with your meals
9. Alcoholic beverages
10. All forms of tobacco
11. Prolonged periods of direct sun exposure
12. NutraSweet and saccharine
Managing Fibromyalgia
In general, treatments for fibromyalgia include both medication and self-care. The emphasis is on minimizing symptoms and improving general health.
Medications
Medications can help managing fibromyalgia pain and improve sleep. Common choices include:
- Analgesics. Acetaminophen (Tylenol, others) may ease the pain and stiffness caused by fibromyalgia. However, its effectiveness varies. Tramadol (Ultram) is a prescription pain reliever that may be taken with or without acetaminophen. Your doctor may recommend nonsteroidal anti-inflammatory drugs (NSAIDs) — such as aspirin, ibuprofen (Advil, Motrin, others) or naproxen sodium (Aleve, others) — in conjunction with other medications. NSAIDs haven't proved to be as effective in managing fibromyalgia pain when taken by themselves.
- Antidepressants. Your doctor may prescribe amitriptyline to help promote sleep. Fluoxetine (Prozac) in combination with amitriptyline is effective in some people. Duloxetine (Cymbalta) may help ease the pain and fatigue associated with FMS. And milnacipran (Savella) was recently approved by the Food and Drug Administration for managing fibromyalgia symptoms.
- Anti-seizure drugs. Medications designed to treat epilepsy are often useful in reducing certain types of pain. Gabapentin (Neurontin) is sometimes helpful in reducing FMS symptoms, while pregabalin (Lyrica) is the first drug approved by the Food and Drug Administration for managing fibromyalgia.
Therapy
- Physical therapy. Specific exercises can help restore muscle balance and may reduce pain. Stretching techniques and the application of hot or cold also may help.
- Counselling. Cognitive behavioural therapy seeks to strengthen your belief in your abilities and teaches you methods for dealing with stressful situations. Therapy is provided through individual counselling, classes, and with tapes, and may help managing fibromyalgia.
- Trigger point injections with lidocaine.
- Acupuncture/acupressure.
- Relaxation/biofeedback techniques
- Osteopathic manipulation.
- Chiropractic care.
- Therapeutic massage.
- Gentle exercise program.
The most important therapy for muscle pain is regular, low-impact exercise. Keeping muscles conditioned and healthy by exercising three times a week decreases the amount of discomfort. It is important to try low-stress exercises such as walking, swimming, water aerobics, and biking rather than muscle-straining exercises such as weight training. Besides helping with tenderness, regular exercises can also boost energy levels and help with sleep.
Other home-care techniques that can help managing fibromyalgia include these:
- heat applied to sore muscles,
- stretching exercises (Pilates is one form of exercise that may be beneficial), and
- massage.
Exercising With Fibromyalgia
Exercise Can Help, it is crucial to get your muscles healthy which can offer some relief. Healthy muscles are flexible, which can increase your range of motion and the stronger you are, the more you can move around each day. Other benefits include:
- Better sleep
- Reduced stress and depression
- Improved your energy levels
- More endurance
- Weight control
Your first order of business is to start SLOWLY. Your goal should be to improve your health (so forget about weight loss for now). Even walking feels like a chore so you may only be able to exercise for minutes at a time. That's normal! Setting small goals (i.e., walk two minutes today and add a minute every day after) can help you slowly increase your exercise time. Other activities you might enjoy are:
- Swimming - This is a great way to condition your heart and body while getting full and gentle support from the water. No impact means your joints are protected.
- Yoga - Increase your flexibility and de-stress by learning how to relax and breathe. Take care to keep movements easy...some postures may be too difficult so talk to your instructor about modifications.
- Tai Chi - This 'moving meditation' helps you get back in touch with your body and stay active without impact or jarring movements.
Cardio is important, and so is strength training. But, before you do anything check with your doctor and get a referral to a physical therapist so you know exactly what to do. In general, strength training exercises for managing fibromyalgia can include:
- Pushups-Do them against a wall instead of on the floor
- Lifting weights-Use very light weights or even canned food for resistance
- Resistance Bands-Use a light resistance and take your time.
- Machines-Make sure you get instructions on how to use them and start with NO weight.
Condition your body slowly and only do as much as you can. Give yourself at least one day (preferably two) of rest before going back to weights.
The hardest part of exercising with FM is the frustration--knowing that you used to be able to do more and now you can barely get out of bed. Try channelling that frustration into your workouts, reminding yourself that every time you move around you are improving. Taking control of your health can provide tremendous relief, not only physically but emotionally.
PHYSIOTHERAPY FOR MANAGING FIBROMYALGIA
The goal of physical therapy is to maximize function and reduce impairment to limit disability in patients with musculoskeletal conditions. (1) Based on a British study, physical therapists most commonly use exercise, education about correct posture and functional activity, relaxation, and energy conservation and fatigue management. (2) For this review, physical therapy is defined as a treatment program that includes patient education and supervised exercise.
- Numerous modalities, including electrotherapy (transcutaneous electrical nerve stimulation), cryotherapy, and therapeutic heat, can reduce pain. Teach patients how and when to use therapeutic modalities as part of their maintenance program.
- One investigator recommends muscle energy treatments, positional release methods, and massage as part of the rehabilitation program to decrease stiffness and pain.
- Some investigators have found that daily aerobic and flexibility exercises are an essential component of the rehabilitation program. Subsequent clinical trials have confirmed the benefits of aerobic exercise and muscle strengthening on mood and physical functioning.
- Patients should begin with gentle warm-up, flexibility exercises and progress to stretching all of the major muscle groups. Low-impact aerobic exercise is necessary at least 3 times weekly. Patients should always start at low levels of exercise and progress slowly. The goal is to exercise safely without increased pain. The patients' target exercise regimen is 4-5 times a week for at least 20-30 minutes each time; this may take the patient months to achieve.
- Some patients with fibromyalgia may never be able to achieve this level of exercise; encourage them to exercise at the highest level possible without worsening their symptoms.
- Some investigators believe that aquatic exercise may be the safest and gentlest aerobic conditioning exercise available for this group. Aquatic therapy enables aerobic conditioning and also flexibility, strengthening, and stretching exercise. Aquatic exercise is well tolerated and is especially helpful for some patients.
According to the American Physical Therapy Association, physical therapists teach self-management skills to people with all types of conditions. That includes people with fibromyalgia. Physical therapists can help managing fibromyalgia by relieving symptoms of pain and stiffness in everyday life. These health care professionals teach people with FMS how to build strength and improve their range of motion. They show them ways to get relief from deep muscle pain. And they can help in managing fibromyalgia by teaching people how to make sensible decisions about daily activities that will prevent painful flare-ups.
Proper posture, which your physical therapist will help you with, allows efficient muscle function. That results in your being able to avoid undue fatigue and pain. In addition, the therapist may use slow stretching exercises to help you improve muscle flexibility. Relaxation exercises that the therapist will show you will help you reduce muscle tension. While there is no known cure for fibromyalgia, physical therapy may help in managing fibromyalgia pain. It can also help reduce stiffness and fatigue. Physical therapists use a wide range of resources to support exercise. These resources range from deep tissue massage to ice and heat packs for hydrotherapy. With these tools, physical therapists can help people with FMS use their muscles, stretch for flexibility, and move their joints through range-of-motion exercises.
The benefit of physical therapy is that it allows a person with fibromyalgia to work closely with a trained professional who can design a fibromyalgia-specific treatment program. The therapist documents your progress and gauges whether you're practicing good therapy habits, alignments, and movement patterns when doing "homework" or exercises at home.
Hydrotherapy with moist heat or cold packs works by stimulating your body's own healing force. For instance, cold compresses reduce swelling by constricting blood vessels. That helps control minor internal bleeding. Conversely, warm, moist compresses on painful areas dilate blood vessels. That increases the flow of blood, oxygen and other nutrients and speeds the elimination of toxins. Thus hydrotherapy also helps in managing fibromyalgia.
References
- Clauw DJ, Arnold LM, McCarberg BH, FibroCollaborative. The science of fibromyalgia. Mayo Clin Proc. 2011;86(9):907-11. [PubMed]
- Chronic Pain & Fatigue Research Center, Department of Anesthesiology, University of Michigan, Ann Arbor, Michigan 48106, USA. Fibromyalgia: an overview. Am J Med. 2009 Dec;122(12 Suppl):S3-S13.
- Wolfe F, Clauw DJ, Fitzcharles MA, Goldenberg DL. Fibromyalgia criteria and severity scales for clinical and epidemiological studies. J Rheumatol. 2011 Jun;38(6):1113-22.
- Fibromyalgia. From Wikipedia, the free encyclopedia
What Other Visitors Have Said
Click below to see contributions from other visitors to this page...
Can EFT Help With Fibromyalgia? 




Emotional Freedom Technique (EFT) was created to help fight stress. Several studies were performed to examine the potency of EFT and many of these concluded …
Electromagnetic Hypersensitivity 




Traditionally the diagnosis of Fibromyalgia is related to environmental illness. It is currently the understanding that there are basically three illnesses …
Return from Managing Fibromyalgia to Home page
Recent Articles
|
Author's Pick
Rating: 4.4 Votes: 252 |

