Enhance your health with free online physiotherapy exercise lessons and videos about various disease and health condition
Femoral neck fracture physiotherapy protocol
Post femoral neck fracture physiotherapy aims to improve strength and range of motion of the involved extremity. Establish independent gait without assistive device and minimize complications.
Objectives
- I. Increase strength of involved extremity to within functional limits.
- II. Improve range of motion to normal functional status.
- III. Establish independent gait without assistive device.
- IV. Provide equipment and posthospital care as necessary.
- V. Coordinate care with other disciplines involved.

Fracture Neck of Femur: Introduction
This is probably the most common and most significant fracture in terms of morbidity, mortality and socioeconomic impact in developed countries (Reginster et al. 1999). Mortality afer fracture neck of femur is high; (Schurch et al. 1996) found that the 1 year death rate was as high as 23.8 percent.
Classifications
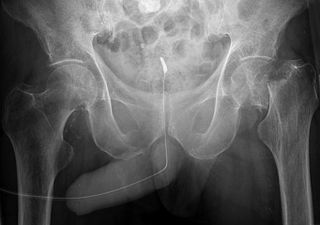
The following is the Garden classification of femoral neck fractures:
- Type 1- inferior cortex is not completely broken.
- Type 2- cortex is broken but there is no angulation.
- Type 3- some displacement and rotation of the femoral head.
- Type 4- complete displacement.
In addition, femoral neck fracture is classified by its location:
- 1. subcapital
- 2. transcervical
- 3. basicervical
- 4. intertrochanteric
- 5. subtrochanteric.
Femoral neck fractures are extremely common in the elderly, often following falls, and most orthopedic units will have a number of these fractures at any one time. The bone's architecture may have been so weakened that patients state they 'heard a crack' before they hit the ground. In other words, the fracture caused the fall, not the fall the fracture. Osteoporosis is often referred to as the silent epidemic as it may not present any clinical signs until fracture.
The resulting fracture is usually displaced with lateral rotation of the femoral shaft so that the leg will be laterally rotated in comparison with the other limb. Occasionally the fragments are impacted in slight abduction and the patient may be able to get up and walk after the injury. Displaced fractures will need operative fixation. The usual method is to excise the head and perform replacement arthroplasty using one of the metal prosthesis e.g. Thompson's hemiarthroplasty. This is the method of choice for displaced fractures because of the dangers of avascular necrosis, and because of the benefits of early mobilization , which is so important in the frail.
An alternative method of fixation is a compression screw plate called a ' dynamic hip screw'- so called because it permits dynamic movement at the fracture site, which stimulates healing. Minimally displaced (e.g. Garden type 1) fractures may be managed by cannulated screw fixation.
Complications:
Main risks following ORIF-
- Non-Union 20-30%
- Avascular Necrosis 10-20%
- Conversion needed 25-30%
Main risks following Arthroplasty-
- Sepsis <5% (mortality >50%)
- Dislocation 4% Hemi, 10% Total
- Re-operation 10%
Reasons for non-union-
- 1. Intra-articular fracture (synovial fluid a deterrent to union)
- 2. Poor vascular supply
- 3. Lacking periosteum & union is endosteal
- 4. Fracture subjected to high shearing forces
- 5. Bone quality may poor
Femoral neck fracture physiotherapy Evaluation
I. Areas to evaluate for femoral neck fracture physiotherapy
A. Postoperative evaluation
1. Two to three days postoperative
- a. Evaluate gross muscle strength and range of motion of other extremities.
- b. Observe gross muscle strength of involved extremity by strength of isometric muscle contractions.
- c. Assess sensation of involved extremity.
- d. Assess range of motion of involved hip within limits of pain.
2. Three to five days postoperative
- a. Evaluate gait pattern with assistive device.
- b. Evaluate functional ability with regard to transfers and bed mobility.
- c. Continue to evaluate gross strength of involved extremity.
B. Outpatient evaluation
- 1. Complete specific muscle tests on all groups.
- 2. Test range of motion of hip, knee, and ankle.
- 3. Analyze gait.
- 4. Evaluate functional ability.
- 5. Complete specific tests, including Functional Ambulation Profile and Get Up & Go Test.
II. Precautions during evaluation
- A. Weight-bearing status must be determined by physician.
- B. Assess cardiac status prior to initiation of evaluation.
Treatment/Goals
Mobilisation after fracture: Femoral neck fracture Physiotherapy
Note
- Required Healing time- 12 to 16 weeks
- Required Rehabilitation time- 15 to 30 weeks
Patients with cemented joint replacements can weight bear as tolerated (WBAT) unless the operative procedure involved a soft-tissue repair or internal fixation of bone.
Patients with cementless, or ingrowth , joint replacements are put on partial weight bearing (PWB) or toe-touch weight bearing (TTWB) for 6 weeks to allow maximum bony ingrowth to take place.
I. Frequency
- A. Inpatients should be seen daily, twice if possible.
- B. Outpatients are followed as necessary.
II. Treatment techniques and goals
A. Two to three days postoperative
- 1. Instruct patient in deep breathing and cough. Goal: Prevent postoperative pneumonia and atelectasis.
- 2. Initiate isometrics and ankle pumps with involved extremity. Goal: Prepare patient for active exercise program.
- 3. Initiate bedside sitting once physician has cleared patient for this activity. Goal: Prepare patient to begin transfer and progressive gait training processes.
B. Three to five days postoperative
- Gait train patient, observing weight-bearing precautions. Progress to walker or crutches. Goal: Establish independent gait with assistive device, using proper gait pattern on all surfaces and stairs.
- Initiate training in activities of daily living, including bed mobility and transfers to and from bed and toilet. Goal: Achieve independence with all transfers.
- Initiate active range of motion/strengthening program. Individualize exercise program according to each patient's needs, but generally include the following. Goals: Increase strength of involved extremity; increase independence with exercise program.
- a. Supine: hip abduction and adduction, gluteal sets, quadriceps sets, straight leg raise, hip and knee flexion, short arc quadriceps, internal and external rotation.
- b. Sitting: Long arc quadriceps, hip flexion, ankle pumps.
III. Equipments
- A. Bilateral support assistive devices (crutches or walker).
- B. Other adaptive equipment as necessary for independence.
IV. General considerations
- A. Evaluate patient's home situation to determine need for additional equipment, home health physical therapy services, or other support.
- B. Request physician consult for necessary equipment or other needs.
Discharge
I. Evaluation. Make final assessment of patient's functional level, gait, range of motion, and strength.
II. Follow-up plan/referral
- A. Continue outpatient physical therapy program as indicated.
- B. Initiate home health physical therapy services when indicated.
III. Home program
- A. Educate patient and family on exercise program.
- B. Provide written home exercise program.
Femoral Neck Fracture Physiotherapy Management in Detail
Femoral neck fracture Physiotherapy Management after Surgery
During the 1st week: Femoral neck fracture Physiotherapy Management
The wound is inspected for evidence of infection and the drains are removed after 24 hours. Pulmonary embolism and hypovolaemia are a distinct possibility and a careful watch is kept to prevent bedsores from developing, the patient is frequently turned in the bed. Derotation bar helps prevent external rotation of the affected limb. Patients treated with hemiarthroplasty should avoid keeping the hip in adduction or internal rotation to prevent redislocation.
a. Movements: A full range active movements of the ankle, gentle active movements of flexion and extension of the hip and knee (once the pain subsides) is permitted. Caution: No passive range of motion at this stage.
b. Exercises: After the pain subsides, isometric gluteal and quadriceps exercises are begun. Isotonic exercises are prescribed for the ankle as it helps to strengthen the gastro-soleus muscle and reduces the chances of thrombophlebitis and deep vein thrombosis.
c. Weight-bearing: By the end of first week, weight bearing with the help of a crutch or walker using a 3-point gait may be permitted. However, it is deferred in unstable fractures. For patients with endoprosthesis, weight bearing as tolerated is permitted.
d. Activities of daily living: Certain modifications are brought about in the activities of daily living. Use of raised toilet seat and chair, wearing the trousers from the affected limb first and removing it from the unaffected limb, rolling on to the unaffected side before getting up from the bed are some of the recommended modifications in daily living.
During 2-4 weeks: Femoral neck fracture Physiotherapy Management
a. Movements: Active and active-assistive movements of the hip, knee and ankle can now be started. However, no passive movements are still recommended.
b. Exercises: Ankle isotonic exercises are continued. Isometric exercises for the hip and knee are prescribed.
c. Weight-bearing: This has to be done on the following lines:
- 1. First the patient is advised prone lying.
- 2. Next as a preclude to weight bearing, four point kneeling is advised.
- 3. Then patient is advised to bear weight on the knees.
- 4. Next, knee walking is encouraged.
- 5. Patient may now be allowed to bear the weight on the affected extremity either partially or fully depending on the stability of the fracture. A 3-point gait using crutches or walker is advised.
d. Activities of daily living: Modifications in activities of daily living are the same as mentioned earlier.
during 4-8 weeks: Femoral neck fracture Physiotherapy Management
The treatment regimen is more or less the same as discussed above. The patient can now flex the hip upto 90 degree, by the self-assisted "heel drag", (i.e. dragging the heel upto the buttocks with the help of the normal leg). The patient can now be encouraged to sit with the legs hanging over the edge of the bed and supporting and lifting the affected limb with the unaffected leg. Assisted and self-resistive exercises for the hip and knee muscles can be carried out.

After 8 weeks: Femoral neck fracture Physiotherapy Management
Passive range of movements by the physiotherapist or by continuous passive motion apparatus is begun to the hip and knee. Isotonic and isokinetic exercises to the hip and knee are initiated alongwith progressive resistive exercises. Weight-bearing with the affected extremity with the help of crutches or walker using a four point gait can be initiated as the patient can bear more weight now. Activities of daily living can be allowed normally with the help of assistive devices.
However, excessive adduction and internal rotation should be avoided in patients treated with endoprosthesis.

By 12-16 weeks: Femoral neck fracture Physiotherapy Management
Full weight-bearing is allowed. Full active and passive range of motion exercises are permitted to the hip and knee joints. Isometrics, isotonic and progressive resistive exercises are continued to the hip, knee and ankle joints. Patient can now carry out all the activities of daily living independently.
The physiotherapy regimen is more or less the same for patients treated with hemiarthroplasty (the emphasis is on to prevent adduction and internal rotation to prevent redislocation), McMurray's osteotomy, Meyer's muscle pedicle graft, etc.
References
- Handoll HHG, Sherrington C. Mobilisation strategies after hip fracture surgery in adults. Cochrane Database of Systematic Reviews 2007, Issue 1.
- Tidy's Physiotherapy15: Tidy's Physiotherapy By Stuart B. Porter
- Essentials of Orthopaedics for Physiotherapist By Ebnezar
- Physical Therapy Protocols Guidelines for Rehabilitation- Edited by Janet Bezner, M.S., PT., and Helen Rogers, M.A., P.T.
- Femoral Neck Fracture- Radiopedia.org
Return from Femoral neck fracture Physiotherapy to Home Page
Recent Articles
|
Author's Pick
Rating: 4.4 Votes: 252 |

