Enhance your health with free online physiotherapy exercise lessons and videos about various disease and health condition
Treatment for COPD
by Prodyut Das
(New Delhi, India)
The pulmonary rehabilitation for treatment of COPD has multidisciplinary team and can consist of a physiatrist and pulmonologist; respiratory, physical, and occupational therapists; an exercise physiologist; a psychiatrist or psychologist; a social worker; a vocational counselor; and a dietitian. However, in the present fiscal environment, an effective small program may have only one specifically trained therapist or nurse under physician supervision.
Treatment for COPD (a review for Physiotherapists)
Diagnosis:
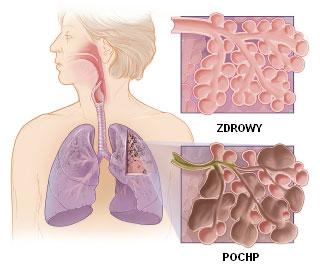
Chronic obstructive pulmonary disease
Medication and Prognosis:
- Favorable, patient on stable self-medication program and non smoking
- Bronchodilators include beta 2-agonists, anticholinergics, and theophyllines
- Other medications, such as corticosteroids, expectorants, mucolytics, and antibiotics, are used along with humidification, ample fluid intake, oxygen therapy and facilitated airway secretion elimination as warranted
Goals:
- Improve endurance and efficiency
- Optimize oxygen needs and control of secretions
- Increase independence in ambulation and self-care activities
- Reduce anxiety and improve self-esteem through enhanced body awareness
Precautions:
- Supplemental oxygen needed during exercise
- Discontinue and notify physician if patients becomes severely dyspneic or develops chest pain with exercise
Respiratory therapy:
- Conduct ear oximetry at rest and during exercise to determine portable oxygen flow rate needed to maintain oxygen saturation higher than 90%
- Instruct patient in diaphragmatic and pursed-lip breathing
- Instruct patient and family in postural drainage techniques
- Instruct patient and family in portable oxygen use
- Instruct in use of metered-dose inhaler before exercise
- Instruct in use of nocturnal bilevel positive airway pressure
Physical therapy:
- Assess baseline endurance, using 12-minute walk test
- Begin incremental exercise program to improve endurance through ambulation and stair climbing. Begin with 5-minute sessions, followed by rest periods between sessions. When patient tolerates 20 minutes of total exercise per day, begin consolidating the sessions.
- Initial treatments on daily basis during weeks 1 and 2, taper to three times per week over weeks 3 and 4, and then taper to home program with self-monitoring in weeks 5 and 6.
- Review proper body mechanics and coordinate with breathing patterns, using diaphragmatic and pursed-lip breathing when appropriate
Occupational therapy:
- Assess upper-extremity mobility, strength, and endurance
- Evaluate basic and advanced self-care activities, and provide adaptive aids to improve independence with dressing, hygiene, bathing, cooking, and other chores
- Train the patient in energy conservation and work simplification techniques
- Evaluate home environment and make recommendations for workspace modifications and equipment to improve safety, efficiency, and independence
- Provide relaxation exercise training with visual imagery techniques
Surgical treatment for severe COPD
- Lung volume reduction surgery
- Lung transplant
Postural Drainage
Disease Emphysema
Chronic Bronchitis
COPD Physiotherapy
Myocardial Infarction Treatment
Lymphedema Physical Therapy
Return to Physiotherapy Discussion Board.