Enhance your health with free online physiotherapy exercise lessons and videos about various disease and health condition
Lateral Femoral Cutaneous Nerve Entrapment (Meralgia Paresthetica)
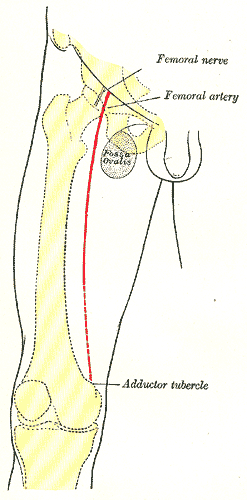
The lateral femoral cutaneous nerve is a sensory nerve, L2 and L3, and is vulnerable to entrapment in the region of the proximal crest of the ASIS, where it passes through the lateral end of the inguinal ligament. The exact site where the nerve exits the pelvis varies. The condition, known as meralgia paresthetica, is characterized by a burning pain in the anterior and lateral portions of the thigh. Pressure over the ASIS usually aggravates the pain.
The mechanism of onset may be traumatic, bur very often the condition is idiopathic. Pelvic tilt or a short leg resulting in postural alterations may be associated with meralgia paresthetica.
Introduction
Meralgia paresthetica (Bernhardt-Roth syndrome) is an entrapment of the lateral cutaneous nerve of thigh that was initially reported to follow operative interventions such as iliac crest bone grafting, appendectomy, pelvic osteotomy, and total abdominal hysterectomy. It is also seen in diabetic and obese patients or in those wearing tight pants, belts, or girdles.
Clinical Features
Most athletes will describe pain, numbness, tingling, and/or burning pain over the anterolateral thigh. Important predisposing factors such as recent weight gain or previous surgical procedure should be obtained. In athletes, prolonged flexion (marksmen), increased muscle mass (weight lifters), or constrictive clothing (tight pant syndrome) may play a role. However, in the athletic population, it is not unusual for no identifiable cause to be found.
Diagnosis
Diagnosis is based on sensory symptoms in the lateral cutaneous nerve distribution. On physical examination, a positive Tinel’s sign is usually present 1 cm medial and inferior to the anterior superior iliac crest. Radiography and MRI of the hip and pelvis are useful to rule out intra-pelvic causes of compression on the nerve and intra-articular derangement. Nerve conduction studies often demonstrate prolonged latency or decreased conduction velocity consistent with compression.
Treatment
Nonoperative treatment is the mainstay of therapy. A local nerve block has been shown to temporarily relieve symptoms and is a useful diagnostic tool and excellent predictor of benefit from surgical decompression . Heat, physical therapy, local steroid injections, and NSAIDs have been shown to be effective. If symptoms are persistent and disabling despite conservative therapy, surgical intervention to perform a nerve decompression may be warranted. Another intervention is transection of the nerve, but this often times results in hypoesthesias and possible neuroma development.
References
- Meralgia paraesthetica. From Wikipedia, the free encyclopedia
- Gregory K. Ivins, MD, FACS. Meralgia Paresthetica, The Elusive Diagnosis. Ann Surg. Aug 2000; 232(2): 281–286. [PubMed]
- Harney D, Patijn J. Meralgia paresthetica: diagnosis and management strategies. Pain Med. 2007 Nov-Dec;8(8):669-77.
- Barna SA, Hu MM, Buxo C, Trella J, Cosgrove GR. Spinal cord stimulation for treatment of meralgia paresthetica. Pain Physician. 2005 Jul;8(3):315-8.
Return from Lateral Femoral Cutaneous Nerve to Home Page
Return from Lateral Femoral Cutaneous Nerve to Orthopedic Physiotherapy
